
نشریه علمی پژوهشی طب انتظامی Journal of Police Medicine

Volume 12, Issue 1 (2023)
J Police Med 2023, 12(1) |
Back to browse issues page
Ethics code: IR.IAU.SDJ.REC.1399.051
Download citation:
BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:



BibTeX | RIS | EndNote | Medlars | ProCite | Reference Manager | RefWorks
Send citation to:
Behzad S, yarahmadi Y, Bahari F, Ahmadian H. Prediction of Addiction Readiness in Cancer Patients Based on the Perception of Social Support with the Mediation of Pain Self-Efficacy and Pain Acceptance. J Police Med 2023; 12 (1)
URL: http://jpmed.ir/article-1-1146-en.html
URL: http://jpmed.ir/article-1-1146-en.html
1- Department of Psychology, Sanandaj Branch, Islamic Azad University, Sanandaj, Iran
2- Department of Psychology, Sanandaj Branch, Islamic Azad University, Sanandaj, Iran ,yyarahmadi@gmail.com
3- Department of Psychology, Arak Branch, Islamic Azad University, Arak, Iran
2- Department of Psychology, Sanandaj Branch, Islamic Azad University, Sanandaj, Iran ,
3- Department of Psychology, Arak Branch, Islamic Azad University, Arak, Iran
English Extended Abstract: (2735 Views)
Aims: Cancer pain creates negative thoughts and beliefs in patients, which can affect the level of functioning and pain tolerance in these patients. In recent decades, the use of drugs for pain relief in cancer patients has increased dramatically. The present study was conducted with the aim of investigating the mediating role of pain acceptance and pain self-efficacy in the relationship between the perception of social support and readiness for addiction.
Materials and Methods: The statistical population of this descriptive-correlation study was men and women with cancer in Arak city in 2020-2021. A total of 201 cancer patients referred to Arak hospitals were selected by available sampling method (97 women and 104 men). Perceived Social Support Questionnaire of Zimet et al. (1988), Pain Self-Efficacy Questionnaire of Nicholas (1980), Chronic Pain Questionnaire of Vowels et al. (2004) and Addiction Readiness Questionnaire by Wade and Butcher (1992) were completed by all the samples. For data analysis, path analysis method was used using SPSS 25 and Amos 24 software.
Findings: Out of 215 participants, 14 were excluded from the analysis due to incomplete completion of the questionnaires, and the final analysis was performed on 201 people. Of these, 104 were men (51.75%), and 97 were women (48.25%). The average age of the participants in the research was 53.46±10.38 years, and 34.82% had a middle school diploma (70 people), 24.37% had a high school diploma (49 people), 30.84% had a bachelor's degree (62 people), and 9.95% had a master's degree or higher (20 people). Nineteen people (9.45%) were single, and 165 (82.08%) were married. Thirty-one (15.4%) of the participants had breast cancer, 29 (14.4%) had prostate cancer, 36 (17.9%) had stomach cancer, 33 (16.4%) had colon cancer, 26 people (12.9%) had bladder cancer, 25 people (12.4%) had skin cancer, nine people (4.5%) had uterine cancer, and 12 people (6.0%) had thyroid cancer. The value of kurtosis and skewness of the variables was in the range of -2 to +2, so the data had a normal distribution and the default of data analysis was followed (Table 1).
There was a negative and significant correlation between the perception of social support and potential for addiction (r=-0.389). Also, there is a positive and significant relationship between the perception of social support and pain acceptance (r=0.486), a positive and significant correlation between the perception of social support and pain self-efficacy (r=0.462), and a negative and significant correlation between pain acceptance and potential for addiction (r=-0.511). Moreover, there was a negative and significant relationship between pain self-efficacy and potential for addiction (r=-0.414).
After descriptive data analysis, path analysis defaults were checked and confirmed. The multicollinearity of the variables was investigated using the tolerance statistic and variance inflation factor, and the results showed no multicollinearity between the variables. Path analysis was used to examine the relationship between the variables of perception of social support, pain acceptance, pain self-efficacy, and potential for addiction. Figure 1 shows the path analysis diagram of the final model, and Table 3 shows the fit indices of the final model in the target sample. The fit indices of the final model include the chi-square index (X²/Df=2.94), comparative fit index (CFI=0.99), incremental fit index (IFI=0.99), Tucker-Lewis fit index (TLI=0.93), and the root mean square deviation of approximation (RMSEA=0.09) indicated the optimal fit of the final model. The results of the direct effect of social support perception on pain acceptance, social support perception on pain self-efficacy, pain acceptance on addiction, and pain self-efficacy on addiction and the standard indirect coefficient of social support perception on addiction with the mediating role of pain acceptance and pain self-efficacy was equal to -0.30 (Table 4). The result of the Sobel test for the significance of the mediating variable of pain acceptance was equal to 3.40 and for the variable of pain efficiency was equal to 2.39. Since the z-value was greater than 1.96, the significance of the influence of mediating variables was confirmed.
Conclusion: Strengthening the social support network of individuals, along with developing a sense of self-efficacy and acceptance of uncontrollable aspects, can be considered as preventive treatment goals and plans for patients' tendency to use drugs for pain relief.
CLINICAL & PRACTICAL TIPS in POLICE MEDICINE
By providing a platform to increase the social network of individuals and by emphasizing holding training courses that are fundamental factors in the formation of an independent and coherent identity when facing life-threatening diseases, psychologists and counselors of military institutions can promote patients’ acceptance and self-efficacy in order to increase the mental health of police forces in the society.
Acknowledgments: We appreciate all the patients who participated in this study.
CONFLICT of INTEREST: The authors stated that there is no conflict of interest in the present study.
AUTHORS CONTRIBUTION: First author, ideation, study design, data collection, data analysis; second author, study design, data collection, data analysis; third and fourth authors, study design and data analysis. All the authors participated in the initial writing of the article and its revision, and all accept the responsibility for the accuracy and correctness of the article's contents with the final approval of this article.
FUNDING SOURCES
This research had no financial support.
Materials and Methods: The statistical population of this descriptive-correlation study was men and women with cancer in Arak city in 2020-2021. A total of 201 cancer patients referred to Arak hospitals were selected by available sampling method (97 women and 104 men). Perceived Social Support Questionnaire of Zimet et al. (1988), Pain Self-Efficacy Questionnaire of Nicholas (1980), Chronic Pain Questionnaire of Vowels et al. (2004) and Addiction Readiness Questionnaire by Wade and Butcher (1992) were completed by all the samples. For data analysis, path analysis method was used using SPSS 25 and Amos 24 software.
Findings: Out of 215 participants, 14 were excluded from the analysis due to incomplete completion of the questionnaires, and the final analysis was performed on 201 people. Of these, 104 were men (51.75%), and 97 were women (48.25%). The average age of the participants in the research was 53.46±10.38 years, and 34.82% had a middle school diploma (70 people), 24.37% had a high school diploma (49 people), 30.84% had a bachelor's degree (62 people), and 9.95% had a master's degree or higher (20 people). Nineteen people (9.45%) were single, and 165 (82.08%) were married. Thirty-one (15.4%) of the participants had breast cancer, 29 (14.4%) had prostate cancer, 36 (17.9%) had stomach cancer, 33 (16.4%) had colon cancer, 26 people (12.9%) had bladder cancer, 25 people (12.4%) had skin cancer, nine people (4.5%) had uterine cancer, and 12 people (6.0%) had thyroid cancer. The value of kurtosis and skewness of the variables was in the range of -2 to +2, so the data had a normal distribution and the default of data analysis was followed (Table 1).
There was a negative and significant correlation between the perception of social support and potential for addiction (r=-0.389). Also, there is a positive and significant relationship between the perception of social support and pain acceptance (r=0.486), a positive and significant correlation between the perception of social support and pain self-efficacy (r=0.462), and a negative and significant correlation between pain acceptance and potential for addiction (r=-0.511). Moreover, there was a negative and significant relationship between pain self-efficacy and potential for addiction (r=-0.414).
After descriptive data analysis, path analysis defaults were checked and confirmed. The multicollinearity of the variables was investigated using the tolerance statistic and variance inflation factor, and the results showed no multicollinearity between the variables. Path analysis was used to examine the relationship between the variables of perception of social support, pain acceptance, pain self-efficacy, and potential for addiction. Figure 1 shows the path analysis diagram of the final model, and Table 3 shows the fit indices of the final model in the target sample. The fit indices of the final model include the chi-square index (X²/Df=2.94), comparative fit index (CFI=0.99), incremental fit index (IFI=0.99), Tucker-Lewis fit index (TLI=0.93), and the root mean square deviation of approximation (RMSEA=0.09) indicated the optimal fit of the final model. The results of the direct effect of social support perception on pain acceptance, social support perception on pain self-efficacy, pain acceptance on addiction, and pain self-efficacy on addiction and the standard indirect coefficient of social support perception on addiction with the mediating role of pain acceptance and pain self-efficacy was equal to -0.30 (Table 4). The result of the Sobel test for the significance of the mediating variable of pain acceptance was equal to 3.40 and for the variable of pain efficiency was equal to 2.39. Since the z-value was greater than 1.96, the significance of the influence of mediating variables was confirmed.
Conclusion: Strengthening the social support network of individuals, along with developing a sense of self-efficacy and acceptance of uncontrollable aspects, can be considered as preventive treatment goals and plans for patients' tendency to use drugs for pain relief.
CLINICAL & PRACTICAL TIPS in POLICE MEDICINE
By providing a platform to increase the social network of individuals and by emphasizing holding training courses that are fundamental factors in the formation of an independent and coherent identity when facing life-threatening diseases, psychologists and counselors of military institutions can promote patients’ acceptance and self-efficacy in order to increase the mental health of police forces in the society.
Acknowledgments: We appreciate all the patients who participated in this study.
CONFLICT of INTEREST: The authors stated that there is no conflict of interest in the present study.
AUTHORS CONTRIBUTION: First author, ideation, study design, data collection, data analysis; second author, study design, data collection, data analysis; third and fourth authors, study design and data analysis. All the authors participated in the initial writing of the article and its revision, and all accept the responsibility for the accuracy and correctness of the article's contents with the final approval of this article.
FUNDING SOURCES
This research had no financial support.
Table 1) Mean, kurtosis and skewness of research variables
| Variable | M±SD | Kurtosis | Skewness |
| Pain acceptance | 45.20±5.78 | 0.97 | 0.38 |
| Pain self-efficacy | 30.66±6.19 | -0.09 | 0.08 |
| Potential for addiction | 76.68±8.03 | -0.04 | -0.060 |
| Perception of social support | 33.38±3.64 | 1.19 | 1.60 |
Table 2) Correlation matrix of research variables
| Variable | 1 | 2 | 3 | 4 |
| Pain acceptance | 1 |
| Pain self-efficacy | 0.448** | 1 |
| Potential for addiction | -0.511** | -0.414** | 1 |
| Perception of social support | 0.486** | 0.462** | -0.389** | 1 |
Significant at the p<0.01 level**
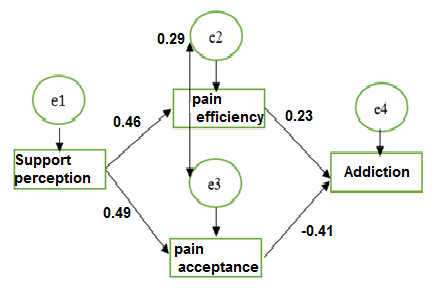
Figure 1) The output model of the role of mediation in the relationship
between the perception of social support and potential for addiction
Table3) final model suitability indices

Figure 1) The output model of the role of mediation in the relationship
between the perception of social support and potential for addiction
Table3) final model suitability indices
| Fit index | Df | X2/Df | RMSEA | CFI | IFI | TLI |
| Acceptable value | + | Less than 3 | Less than 0.10 | More than 90 | More than 90 | More than 90 |
| The final model | 1 | 2.94 | 0.09 | 0.99 | 0.99 | 0.93 |
Table 4) The effect of direct and indirect relationship in the final model
| Direction | Standard beta | p |
| Perception of social support >>> acceptance of pain | 0.48 | 0.001 |
| Perception of social support >>> pain self-efficacy | 0.46 | 0.001 |
| Acceptance of pain >>> potential for addiction | -0.40 | 0.001 |
| Pain self-efficacy >>> potential for addiction | -0.23 | 0.001 |
| Perception of social support >>> pain acceptance* pain self-efficacy >>> addiction | -0.30 | 0.001 |
Keywords: Addiction [MeSH], Cancer Pain [MeSH], Social Support [MeSH], Self-Efficacy [MeSH], Pain [MeSH]
Article Type: Original Research |
Subject:
Police Related Psychology
Received: 2022/10/24 | Accepted: 2023/01/7 | Published: 2023/02/17
Received: 2022/10/24 | Accepted: 2023/01/7 | Published: 2023/02/17
References
1. Higginson IJ, Costantini M. Dying with cancer, living well with advanced cancer. Eur J Cancer. 2008;44(10):1414-24. [DOI:10.1016/j.ejca.2008.02.024] [PMID]
2. Daher M. Opioids for cancer pain in the Middle Eastern countries: a physician point of view. J Pediatr Hematol Oncol. 2011;33(1):23-8. doi: 10.1097/MPH.0b013e3182121a0f [DOI:10.1097/MPH.0b013e3182121a0f] [PMID]
3. Mousavi SM, Pourfeizi A, Dastgiri S. Childhood cancer in Iran. J Pediatr Hematol Oncol. 2010;32(5):376-82. doi: 10.1097/MPH.0b013e3181e003f7 [DOI:10.1097/MPH.0b013e3181e003f7] [PMID]
4. Sandblom G, Carlsson P, Sennfält K, Varenhorst E. A population-based study of pain and quality of life during the year before death in men with prostate cancer. Br J Cancer. 2004;90(6):1163-8. [DOI:10.1038/sj.bjc.6601654] [PMID] [PMCID]
5. Gupta S, Atcheson R. Opioid and chronic non-cancer pain. J Anaesthesiol Clin Pharmacol. 2013;29(1):6-12. doi: 10.4103/0970-9185.105784 [DOI:10.4103/0970-9185.105784] [PMID] [PMCID]
6. Carmichael AN, Morgan L, Del Fabbro E. Identifying and assessing the risk of opioid abuse in patients with cancer: an integrative review. Subst Abuse Rehabil. 2016;7:71-9. doi: 10.2147/SAR.S85409 [DOI:10.2147/SAR.S85409] [PMID] [PMCID]
7. Turk DC, Melzack R. Handbook of pain assessment: Guilford Press. 3rd ed. 2010. 542p. https://www.guilford.com/books/Handbook-of-Pain-Assessment/Turk-Melzack/9781606239766
8. Holtzman S, Newth S, Delongis A. The role of social support in coping with daily pain among patients with rheumatoid arthritis. J Health Psychol. 2004;9(5):677-95. [DOI:10.1177/1359105304045381] [PMID]
9. Meredith P, Ownsworth T, Strong J. A review of the evidence linking adult attachment theory and chronic pain: presenting a conceptual model. Clin Psychol Rev. 2008;28(3):407-29. [DOI:10.1016/j.cpr.2007.07.009] [PMID]
10. Solaro C, Brichetto G, Amato MP, Cocco E, Colombo B, D'Aleo G et al. The prevalence of pain in multiple sclerosis: a multicenter cross-sectional study. Neurology. 2004;63(5):919-21. [DOI:10.1212/01.WNL.0000137047.85868.D6] [PMID]
11. Burleson JA, Kaminer Y. Self-efficacy as a predictor of treatment outcome in adolescent substance use disorders. Addict Behav. 2005;30(9):1751-64. [DOI:10.1016/j.addbeh.2005.07.006] [PMID]
12. Naar-King S, Wright K, Parsons JT, Frey M, Templin T, Ondersma S. Transtheoretical model and substance use in HIV-positive youth. AIDS Care. 2006;18(7):839-45. [DOI:10.1080/09540120500467075] [PMID]
13. Jensen MP, Smith AE, Alschuler KN, Gillanders DT, Amtmann D, Molton IR. The role of pain acceptance on function in individuals with disabilities: a longitudinal study. Pain. 2016;157(1):247-54. doi: 10.1097/j.pain.0000000000000361 [DOI:10.1097/j.pain.0000000000000361] [PMID]
14. Van Damme S, Crombez G, Eccleston C. Coping with pain: a motivational perspective. Pain. 2008;139(1):1-4. [DOI:10.1016/j.pain.2008.07.022] [PMID]
15. Lee EB, An W, Levin ME, Twohig MP. An initial meta-analysis of acceptance and commitment therapy for treating substance use disorders. Drug Alcohol Depend. 2015;155:1-7. [DOI:10.1016/j.drugalcdep.2015.08.004] [PMID]
16. Denison E, Asenlöf P, Sandborgh M, Lindberg P. Musculoskeletal pain in primary health care: subgroups based on pain intensity, disability, self-efficacy, and fear-avoidance variables. J Pain. 2007;8(1):67-74. [DOI:10.1016/j.jpain.2006.06.007] [PMID]
17. Davis MI, Jason LA. Sex differences in social support and self-efficacy within a recovery community. Am J Community Psychol. 2005;36(3-4):259-74. [DOI:10.1007/s10464-005-8625-z] [PMID]
18. Damirchi ES, Fayazi M, Mohammadi N. The relationship between self-efficacy and perceived social support with addiction tendency among soldiers. J Mil Med. 2017;18(4):316-24. http://militarymedj.ir/browse.php?a_id=1489&sid=1&slc_lang=en&ftxt=1
19. Azad Marzabadi E, Fathi Ashtiyani A, Ahmadi Zade MJ, Anisi J, Ziaee M. Study the relationship between social support and self-efficacy in staffs of one of the military organizations. Journal of Police Medicine. 2015;4(1):57-64. http://jpmed.ir/article-1-185-fa.html
20. Lin LA, Bohnert AS, Price AM, Jannausch M, Bonar EE, Ilgen MA. Pain acceptance and opiate use disorders in addiction treatment patients with comorbid pain. Drug Alcohol Depend. 2015;157:136-42. [DOI:10.1016/j.drugalcdep.2015.10.017] [PMID]
21. Manne SL, Kashy DA, Virtue S, Criswell KR, Kissane DW, Ozga M, et al. Acceptance, social support, benefit-finding, and depression in women with gynecological cancer. Qual Life Res. 2018;27(11):2991-3002. [DOI:10.1007/s11136-018-1953-x] [PMID] [PMCID]
22. Zimet GD, Powell SS, Farley GK, Werkman S, Berkoff KA. Psychometric characteristics of the multidimensional scale of perceived social support. J pers Assess. 1990;55(3-4):610-7 [DOI:10.1080/00223891.1990.9674095] [PMID]
23. Salimi A, Joukar B, Nikpour R. Internet and communication: Perceived social support and loneliness as antecedent variables. 2009;11(3):23-35. [Persian]. https://www.sid.ir/paper/67702/en
24. Nicholas MK. The pain self-efficacy questionnaire: taking pain into account. European journal of pain. 2007;11(2):153-63. [DOI:10.1016/j.ejpain.2005.12.008] [PMID]
25. Asghari A, Nicholas MK. Pain self-efficacy beliefs and pain behaviour. A prospective study. Pain. 2001;94(1):85-100. [DOI:10.1016/S0304-3959(01)00344-X] [PMID]
26. McCracken LM, Vowles KE, Eccleston C. Acceptance of chronic pain: component analysis and a revised assessment method. Pain. 2004;107(2):159-66. [DOI:10.1016/j.pain.2003.10.012] [PMID]
27. Meskarian F, Moghaddam M, Shaeiri M. The relation between acceptance of pain and reduced pain intensity and disability among chronic pain patients. Behav Res. 2012;10(3):67-74.20.1001.1.17352029.1391.10.3.5.3
28. Weed NC, Butcher JN, McKenna T, Ben-Porath YS. New measures for assessing alcohol and drug abuse with the MMPI-2: The APS and AAS. J Pers Assess. 1992;58(2):389-404. [DOI:10.1207/s15327752jpa5802_15] [PMID]
29. Zargar Y, Najarian B, Naami A. The relationship of some personality variables, religious attitudes and marital satisfaction with addiction potential in personnel of an industrial factory in Ahvaz. Edu J. 2008;15(1):99-120. [Persian]. https://www.magiran.com/paper/1828010?lang=en
30. Setayeshi Azhari M, Mirzahosseini H, Mohebi M. The relationship between perceived support and readiness for addiction and psycchological distress with the mediating role of loneliness in students. Addict Res. 1397;12(46):157-72. [Persian]. https://www.sid.ir/paper/113625/en
31. Massah O, Azkhosh M, Azami Y, Goodiny AA, Doostian Y, Mousavi SH. Students tendency toward illicit drug use: The role of perceived social support and family function in Iran. Iranian J Psychiatry Behav Sci. 2017;1(2) :12-31. doi: 10.17795/ijpbs.8314 [DOI:10.17795/ijpbs.8314]
32. Hayes SC, Luoma JB, Bond FW, Masuda A, Lillis J. Acceptance and commitment therapy: model, processes and outcomes. Behav Res Ther. 2006;44(1):1-25. [DOI:10.1016/j.brat.2005.06.006] [PMID]
Send email to the article author
| Rights and permissions | |
 |
This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License. |

